A Snowfall, A Slip… and Sudden Paralysis
A Story of Cervical OPLL, Trauma, and Hope
What began as a joyful holiday in the hills of Shimla turned into a life-altering moment within seconds. He had travelled there to enjoy the snow — laughter, photographs, snow games. Like many others, he slipped while playing. It seemed like a simple fall. But when he tried to get up… he couldn’t.
He was unable to move his arms.
He was unable to move his legs.
Soon after, he lost control over his bowel and bladder.
In the blink of an eye, an active and healthy man was rendered completely paralyzed.

The Week That Changed Everything
Due to the location and logistical challenges, he reached us one week after the injury. When I first saw him, he lay still — completely dependent, frightened, and unsure of what his future held.
On examination, he had:
- Paralysis of all four limbs
- He was wearing diaper and had urinary catheter (beacuse he had no control over his stools or urine)
For any spine surgeon, this is one of the most devastating presentations to encounter.
The Hidden Problem: OPLL
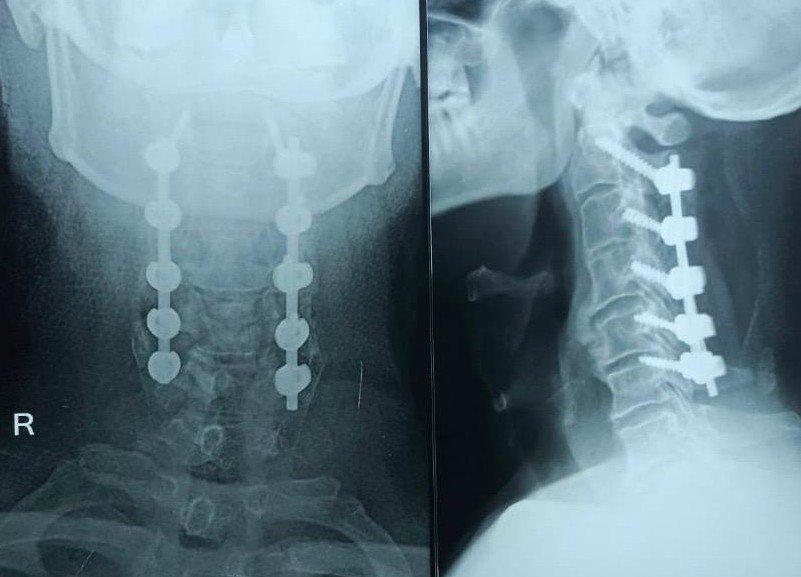
His scans uncovered the reason why a seemingly minor fall resulted in a catastrophic injury. He had extensive Ossified Posterior Longitudinal Ligament (OPLL) from C2 to C6 — a condition where a ligament inside the spinal canal slowly turns into bone. Over time, this had already severely narrowed his spinal canal. The spinal cord was living in a critically tight space. The fall did not just injure him — it was the final trigger in a spine that had no reserve space left.

The Surgical Decision
In cases like this, every minute matters — but even after a week, decompression can still make a difference. We planned an urgent: C2–C6 Laminectomy with Lateral Mass Fixation
The goals were clear:
- Relieve pressure on the spinal cord
- Give the cord space to breathe
- Stabilize the spine
- Prevent further damage
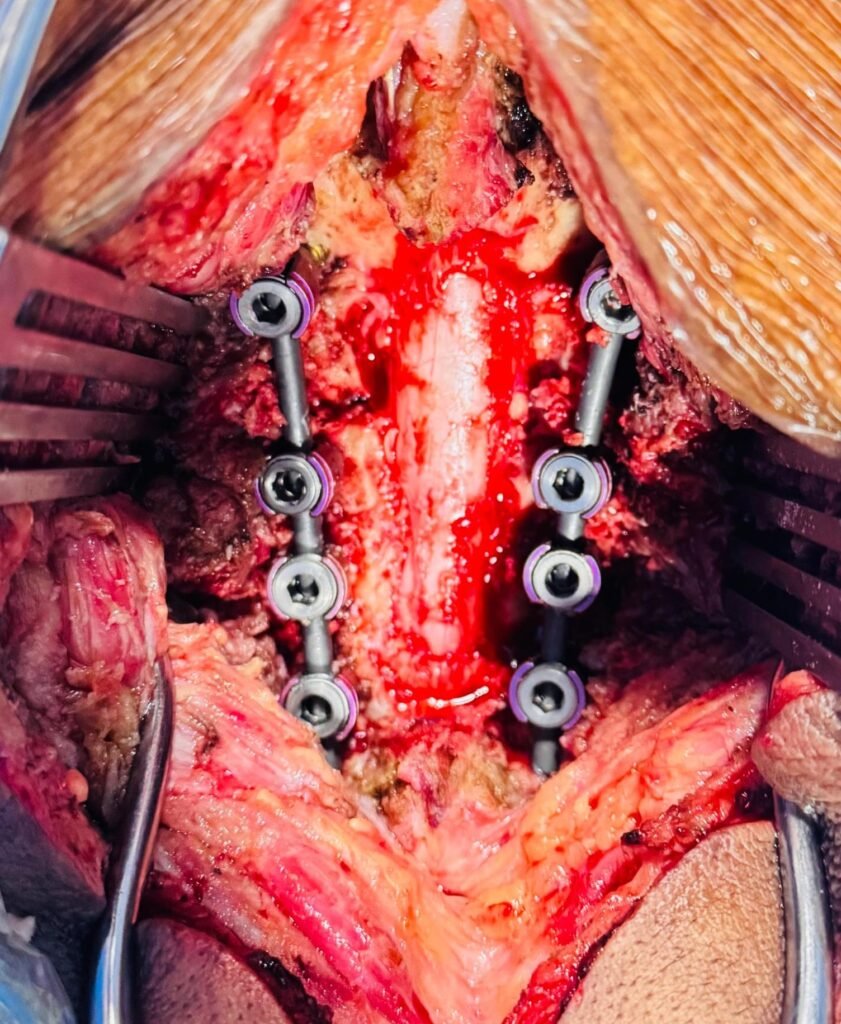
The surgery was meticulous. The compression was severe. The cord was under obvious stress. Once decompressed, the spinal cord slowly expanded posteriorly — a moment every spine surgeon hopes for in such cases.
The Emotional Side of Spine Surgery
Behind every scan is a person. Behind every surgery is a family waiting outside the OT doors. His relatives asked the question we hear so often: “Will he walk again?”
In spinal cord injuries, the answer is never absolute.
Recovery depends on:
- Severity of initial injury
- Cord signal changes
- Timing of decompression
- Postoperative rehabilitation
But what we can always offer is the best possible chance.
The Moment That Changed Everything
The next morning, we assessed him carefully. He was able to move his all four limbs without any assistance. We encouraged him. Supported him. And then — We made him sit.
Then stand.
And then, with assistance…
He took steps.
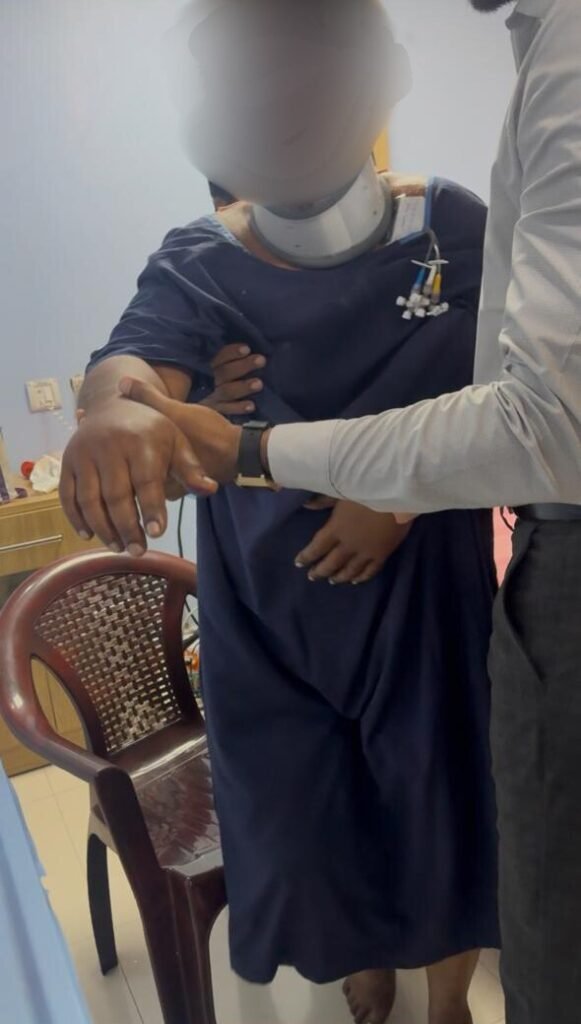
The same patient who arrived unable to move all four limbs – stood up and walked the very next day. For a spine surgeon, these are the moments that define why we do what we do. For the patient and family, it was nothing short of miraculous.
Why Did He Recover?
Several factors may have helped:
- Early surgical decompression (even after 1 week)
- Likely cord edema rather than irreversible myelomalacia
- Effective posterior decompression allowing cord drift
- Immediate mobilization and aggressive rehabilitation
Spinal cord injuries are unpredictable — but when decompression is timely and adequate, the cord can surprise us.
The Bigger Message
- OPLL can remain silent for years.
- Minor trauma can cause catastrophic neurological injury in stenosed canals.
- Early recognition and surgical decompression can dramatically alter outcomes.
- Never underestimate the recovery potential of the spinal cord.
A Reminder to Everyone
If you experience:
- Hand clumsiness
- Difficulty with fine motor tasks
- Neck stiffness with imbalance
- Electric shock sensations in arms or legs
Seek evaluation early.
Sometimes the warning signs are subtle — until they’re not.
–This article is for educational purposes and reflects clinical experience in managing complex cervical spine injuries.
– Dr. Ganesh Kumar, MBBS, MS (Orthopaedics), Post-doctoral Fellowship in Spine Surgery, FASSI(New Delhi).

